Nurse Magnet Recognition at Lexington
Contributions of Professional Nursing at Baptist Health Lexington
Baptist Health Lexington is a five-time consecutively designated Magnet® facility through the American Nurses Credentialing Center (ANCC), which is the highest recognition for nursing excellence worldwide. The Magnet® designation was first achieved at Baptist Health Lexington 2005. Serving as a model of nursing excellence in 2018, Baptist Health was the first community hospital system to have both Magnet® or Pathway to Excellence® credentials at all nine facilities. Supporting the Baptist Health mission, vision and values, the Magnet® credential shows the excellent level of work from nursing. It also confirms the commitment and contributions of nursing at all levels to sustain excellence in professional practice, care delivery and health outcomes. Nurses continually strive to raise the bar of professional practice through individual and group contributions by:
- Having higher levels of nursing education;
- Obtaining nursing certifications;
- Publishing nurse-led and co-led research studies and quality initiatives in peer reviewed journals; and
- Volunteering in community outreach programs and population health initiatives at the local, regional, and state level.
These contributions describe the culture of nursing within the facility, and the resolve of nursing staff to provide the highest quality patient and family-centered care.
Advancing Higher Levels of Nursing Education
In 2010, the Institute of Medicine made a national goal for all healthcare organizations that involved 80% of nursing staff to have a baccalaureate degree (or higher) in nursing (IOM, 2011). Higher levels of education improves the ability of nurses to meet demands of the current healthcare system and improve patient care results. To meet this goal, Baptist Health Lexington provides resources to support nurses returning to college programs. Through monies provided for tuition and use of flexible scheduling, a large volume of RNs and LPNs have advanced their educational to the baccalaureate, master’s, and doctorate level over the past several years. As of the end-year 2024, 72.2% of all RNs earned a baccalaureate degree or higher (see Figure 1).
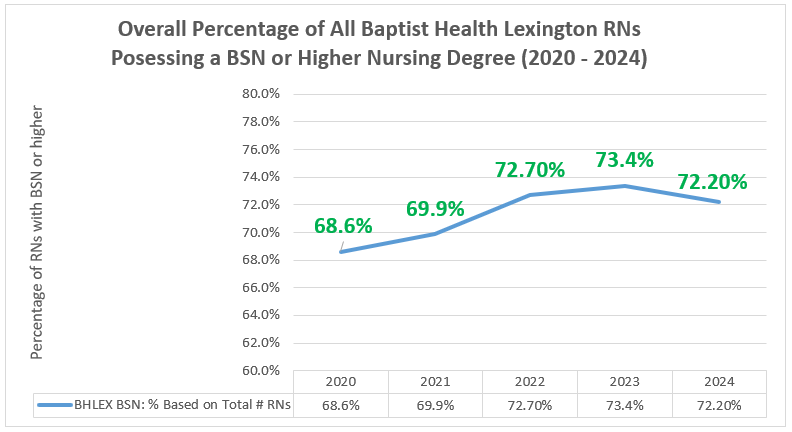
Figure 1. Overall Percentage of BHLEX RNs Possessing a BSN of Higher Degree
Obtaining National Nursing Certifications
We provide resources—both internal and external—to help nurses pursue national specialty certifications. Specialty credentials reflect advanced knowledge and skills, and they contribute to higher patient safety and quality outcomes. As of end-2024, 288 nurses at Baptist Health Lexington have achieved or maintained national certification.
| Name of National Nursing Certification | Certifying Body | Credential |
|---|---|---|
| Critical Care RN with Cardiac Medicine Subspecialty | American Association of Critical Care Nurses (AACN Certification Corporation) | CCRN-CMC |
| Critical Care RN with Cardiac Surgery Subspecialty | American Association of Critical Care Nurses (AACN Certification Corporation) | CCRN-CSC |
| Progressive Care Nursing (Adult) | American Association of Critical Care Nurses (AACN Certification Corporation) | PCCN® |
| Certified Heart Failure Nurse | American Association of Heart Failure Nurses | CHFN |
| Certified Gastrointestinal Registered Nurse | American Board for Certification of Gastroenterology Nurses, Inc. | CGRN |
| Accredited Case Manager | American Case Management Association | ACM |
| Certified Corrections Nurse | American Correctional Association Certification Program | CCN |
| Adult Psychiatric & Mental Health Nurse Practitioner | American Nurses Credentialing Center (ANCC) | PMHNP-BC |
| Cardiac/Vascular Nurse | American Nurses Credentialing Center (ANCC) | CV-BC |
| Nurse Executive | American Nurses Credentialing Center (ANCC) | NE-BC |
| Nurse Executive, Advanced | American Nurses Credentialing Center (ANCC) | NEA-BC |
| Medical-Surgical Registered Nurse | American Nurses Credentialing Center (ANCC) | MEDSURG-BC |
| Family Nurse Practitioner | American Nurses Credentialing Center (ANCC) | FNP-BC |
| Nursing Case Management | American Nurses Credentialing Center (ANCC) | CMGT-BC |
| Stroke Certified Registered Nurse | American Board of Neuroscience Nursing | SCRN |
| Electronic Fetal Monitoring | National Certification Corporation for Obstetric, Gynecologic, and Neonatal Nursing Specialties | C-EFM |
| Certified Healthcare Simulation Educator | Society for Simulation in Healthcare | CHSE |
| Acute/Critical Care Nursing (Adult) | American Association of Critical Care Nurses (AACN Certification Corporation) | CCRN® |
| Acute/Critical Care Nursing (Neonatal) | American Association of Critical Care Nurses (AACN Certification Corporation) | CCRN® |
| Acute Critical Care Knowledge Professional (Adult) | American Association of Critical Care Nurses (AACN Certification Corporation) | CCRN-K™ |
| Pediatric Primary Care Nurse Practitioner | American Nurses Credentialing Center (ANCC) | PPCNP-BC |
| Certified Hospice and Palliative Nurse | Hospice and Palliative Credentialing Center | CHPN® |
| Adult-Gerontology Clinical Nurse Specialist-Board Certified | American Nurses Credentialing Center (ANCC) | AGCNS-BC |
| Nursing Professional Development Certification | American Nurses Credentialing Center (ANCC) | NPD-BC |
| Certified Bariatric Nurse | American Society for Metabolic and Bariatric Surgery | CBN |
Nursing Publications in Peer-Reviewed Journals
Our nurses engage in research and publish findings that advance practice and improve patient care. Coordinated by the Nursing & Allied Health Research Office, these efforts span from associate to doctoral‐prepared clinicians, and leverage our Medical Library and Institutional Review Board support. Since 2008, our team has disseminated 118 scholarly publications, cited by experts in 46 states and 69 countries.
Table 2: Baptist Health Lexington Publications from Nursing & Members of the Healthcare Team (2008-24)
2024
Cruise, K., Walton, J., Monroe, M., Davies, C.C. Evaluation of Class for Environmental Services
Employees for whom English is a Second Language. Nursing Management. Accepted
December 2024.
Monroe, M., Davies, C.C., Bowles, L, Byrd, S., Ford, C. (2024). Buy-in among Mother-Baby Nurses
regarding an Enhanced Recovery after Surgery Protocol. Nursing Management, 55(11): 28-33.
Winner, R., Graves, J., Jarvis, K., Beckman, D., Youkilis, B., Monroe, M., Davies, C.C. (2024). The
relationship between onset of labor and mode of birth. Journal of Obstetric, Gynecologic,
and Neonatal Nursing, 53(5): 503 -510.
Blair K., Thompson M., Mijatovic O., Monroe, M., Davies, C.C. (2024). Evaluation of Delays in the
Operating Room. Journal of Nursing Administration, 54(9): 503-506.
Spagnoli, M., Monroe M., Davies, C. C. (2024). The Effect of Spinning Babies® Education on Confidence
In Implementing Techniques and Knowledge Regarding Safety Related to Labor Positioning
Among Birth Professionals. Journal of Perinatal Education. DOI: 10.1891/JPE-2023-0021.
Kramer, M., Hayden, M., Hovermale, R., Jones, A., Miller, B., Miniard, S.J., Ponder, J., Davies, C.C.,
Monroe, M. (2024). The Effect of a Suicide Prevention Program on Understanding and Beliefs Among Nurses. Journal of Nursing Administration, 54(5): 299- 303.
2023
Smith, M., Rogers, A., Fultz, J., Davies, C.C., Monroe, M. (2024) Assessing factors associated with
Burnout among nurse preceptors. Journal of Nursing Administration, 54(4): 235- 239.
Edwards, J., Bevans, T., Brockopp, D. (2023). The role of a transitional pain approach to surgical care in
A patient with an opioid use disorder: A case report. Journal of Addictions Nursing. Accepted
November 2023.
Hobbs, K., Workman, C., Campbell, S., Coulter, S., Wheeler, P., Monroe, M., Davies, C.C. (2024).
Difference in length of time from biopsy to surgery following genetic counseling. Clinical Journal
of Oncology Nursing, 28(2): 157-16.
Lewis, P., Slyh, A., Robertson M.E., Schenkenfelder, R., Gallivan, T et al. (2023) Development and
evaluation of the Baptist Health Acquired Pressure Injury Risk Assessment Instrument. Journal of
Nursing Administration, 53(9): 438-444.
2022
Davies, C.C., Monroe, M., Brockopp, D., Beckman, D. (2022). Challenges as an Increasing Number of
Nurses Seek Graduate Degrees – Editorial in the Clinical Nurse Specialist Journal. 283-284.
Wheeler, P., Barron, K., Koepke, N., LeMaster, T., Myers, S., Ryan, J., Stinnett, K., Yackzan, S., Monroe,
M., Davies, C.C. Difference in Patient Satisfaction with Postoperative Bras and Drain Securement Methods Among Women Undergoing Mastectomy. Accepted Nursing Management.
Hobbs, K., Davies, C.C., Monroe, M. The effect of an educational intervention on nurse knowledge
of medication management for acute pain crises in patients with cancer. JONS Essentials, 26 (5); 559 – 563.
Glass, A., Monroe, M., Davies, C.C. Influence of a multidisciplinary STOMA team approach on distress,
anxiety, self-efficacy, and patient satisfaction. Journal of Oncology Navigation and Survivorship, 13 (7).
Bowles, L.A, Heet, W., Waterbeck, J., Chastain, L., Monroe, M., Davies, C.C. (2022). The effect of an
Enhanced Recovery after Surgery Protocol on Opioid Consumption, Pain, and Length of Stay among Patients Undergoing Prostatectomy and Nephrectomy. Journal of Perioperative Nursing, 35(2):e-27-e-31.
Monroe, M., Davies, C.C., Brockopp, D., Beckman, D., Cantrell, D. (2022) COVID 19: The lived
experience by Chief Nursing Officers. Journal of Nursing Administration, 52(5); 309-313.
2021
Farmer, M., Monroe, M., Davies, C.C. (2021). Nurses’ knowledge of Alpha-gal allergies. Nursing
Management. 1;52 (12):6-8. doi: 10.1097/01.NUMA.0000800396.67224.8f
Kjelland, K., Allen, M., Holder, K., Jenny, A., Row, C., Troutman, H., Nieves, H., Voils, T., Monroe, M.
(2021). The Tiered Skills Acquisition Model: Orientees’ perception of preceptor performance Nursing Management, 52(9):51-53.
Kramer, M., Fultz, J., Smoot B., Sutherland, S., Wells, N., Monroe, M., Davies, C.C. (2021). Educating
Nurses during a Pandemic to Manage Ventilators. Journal of Nurses in Professional Development, 38(5): E49 – 54.
Kramer, M., Davies, C.C. (2021). The Development of an Effective Charge Nurse Program. Journal of
Nurses in Professional Development, 37(5):268-277. doi:
10.1097/NND.0000000000000765
Brockopp, D., Monroe, M., Davies, C. C., Cawood, M., Cantrell, D. (2021). COVID-19: The Lived
Experience of Critical Care Nurses. Journal of Nursing Administration, 51(7/8):372-378.
Monroe, M., Linares A.M., Ashford, K. (2021). Mothers’ perception of hospital-based care: The effect on
exclusive breastfeeding. Nursing for Women’s Health, 25(4): 257-263.
Rogers, A., Fultz, J., Clements-Hickman, A., Davies, C.C. (2021). The Baptist Health Lexington Nursing
Orientation Progression Tool: A Methodological Study. Journal of Nursing Administration,
51(9):439-447.
A.J. Walid., Edwards, J., Yackzan, S., Stanifer, S., Monroe, M., Brockopp, D., Dollar, S., Self, B., Shearin,
H., Young, T.J. (2021) Reduction in opioid consumption, pain and antiemetic use following used
of an Enhanced Recovery After Surgery protocol for breast cancer patients undergoing
mastectomy. Annals of Breast Surgery, 5;15.
Merritt, S., Kramer, M., Monroe, M., Davies, C.C. (2021). Conducting a Virtual Research Symposium:
Path to Success. Journal of Nursing Administration, 51(5), 240-241.
McGuire, M., Olivo, A., Yackzan S. Productivity measures; Empowering oncology nurse practitioners to
understand and demonstrate value in practice. (2021) Clinical journal of Oncology Nursing. 25(3):247-250.
2020
Bucher, T., Davies, C. C., Clements-Hickman, A., Weaver, C., Breakall, A., & Yackzan, S. (2021). The
effect of education on caregivers’ knowledge and attitudes regarding the use of hand massage, breathing techniques and essential oils in the hospice and palliative care patient population. Nursing Forum, 56(2), 249-254. doi.org/10.1111/nuf.12529
Hands, K., Davies, C. C., Monroe, M., & Brockopp, D. (2021) The Effect of Hospital Pre-birth Classes on
Birth Outcomes. Journal of Perinatal Education, 30(4):196-202. doi: 10.1891/J-PE-D-20-00050.
Workman, C., Davies, C. C., Arthur, C., Martin, D., Ogle, K., Thompson, K., Modawell, K., Tussey, K., &
Morse, L. A. (2020). Evaluation of a multi-site nurse let mobility plan. Journal of Nursing Administration, 50(12), 649-654.
Weaver, C., Davies, C. C., Yackzan, S., Herron, R., & Nettro, A. (2021) Essential Oils Use with Breast
Imaging: A Pilot Study. Journal of Holistic Nursing, 39(2):108-115.
Hobbs, K. B., & Yackzan, S. (2020). Adrenal Insufficiency: Immune Checkpoint Inhibitors and Immune-
Related Adverse Event Management. Clinical Journal of Nursing, 24(3), 240-243.
DOI:10.1188/20.CJON.240-243.
Nieves, H., Clements-Hickman, A., & Davies, C. C. (2021). Effect of a Parent Empowerment Program on LOS, Parental Stress, Patient Satisfaction and Maternal Depression. Journal of Perinatal and Neonatal Nursing, 35(1),92-99.
Kjelland, K., Monroe, M., Moore, T., Cooper, H., & Davies, C. C. (2020). Skin to skin contact following
Cesarean birth, a designated nurse: An evaluation of clinical outcomes and cost. Nursing
Management, 51(7), 8-10.
Harris, P., Lewis, P.C., Graystone, R. (2020). Set Up For Success. How the Pathway to Excellence®
Framework supports ambulatory care nurses. Nursing Management, 51(12), 6-9.
Nelson-Brantley, H.V., Beckman, D., Parchment, J., Smith-Miller, C.A., Weaver, S.H. (2020). Magnet®
and Pathway to Excellence® Focusing on Research and Evidence-based practice. JONA, 50(5), 245-247.
Lewis, C.P., Colcord, K., Peterson, A., Pfister, C., Robertson, M.E., Slyh, A., Smoot, B., Tussey, K., &
Whalen, H. (2020). “C.A.R.E. to Prevent Medical Device Related Pressure Injuries?” American Nurse Journal, Accepted October 2020.
2019
Edwards, J., Dollar, S., Young, T., & Brockopp, D. (2019). The Role of an Acute Pain Service in
Preventing New Persistent Opioid Use Following Surgery. Journal of Nursing Administration,
50(4), 1-5.
Hands, K., Clements-Hickman, A., Brockopp, D., & Davies, C. C. (2019). The Effect of Hospital Pre-birth
Classes on Women’s Birth Preferences and Fear of Childbirth: A Pre and Post-Class Survey. Journal of Perinatal Education, 29(3),134-142.
Walker, M., Fultz, A., Davies, C. C., & Brockopp, D. (2019). Symptoms Experience by MR Technologists’
Exposed to Static Magnetic Fields. Radiologic Technology, 91(4), 316-323.
Bowles, L, Curtis, J, Davies, C, Lengerich, A, Bugajski, A. (2019). The Effect of Music on Mood,
Motivation and Exercise Among Patients in a Cardiac Rehabilitation Program: A Pilot Study.
Nursing Forum. 54(3), 340-344.
Lewis, CP. ANCC Recognition of Professional Nursing Practice. (2019). Recognition Benefits Organizations, Nurses, and Patients. American Nurse Today 14(5), 44-47.
Lewis, CP., Johnson, BH, Donnell, C., Phillips T., Jackson, D., Backus, M.,… Wentz, A. (2019) How One Healthcare System Became the First in the World to Achieve a Combination of Magnet® Recognition and Pathway to Excellence® Designation For All of its Hospitals. Nursing Management, 50 (7), 38-44. doi: 10.1097/01.NUMA.0000558524.37370.ce
Yackzan, S., Stanifer, S., Barker, S., Blair, B., Glass, A., Weyl, H., Wheeler, P. (2019). Outcome
Measurement: Patient Satisfaction Scores and Contact with Oncology Nurse Navigators. Clinical
Journal of Oncology Nursing 23(1), 76-81.
2018
Tussey, K., Yackzan, S., & Davies, C.C. (2018). Moving into a New Hospital Tower: The MOVEE Model.
Nursing Management, 49(12), 12-16.
Wright, L. & Brockopp, D. (2018). Developing a Research Friendly Environment: The Librarian’s Role.
Journal of Nursing Administration, 48(11), 540-541.
Brockopp DY. (2018). Nursing Research: A Conundrum. Journal of Nursing Administration. 48(5):231-232.
Davies, CC, Lengerich A, Bugajski A, Brockopp D. (2018). Detecting Change in Activity Using the Patient-
Specific Functional Scale with Breast Cancer Survivors. Rehabilitation Oncology, 36(2), 117-122.
Fultz, A., Walker, M., Lengerich A., Bugajski, A. (2018). Radiologic Technologists’ Job Satisfaction, Radiologic Technology, 89(6), 536-540.
Winner-Stoltz, R, Lengerich, A, Hench, A J, O’Malley, J, Kjelland, K, Eal, M. (2018). Staff Nurse
Perceptions of Open Pod and Single Family Room NICU Designs on Work Environment and
Patient Care. Advances in Neonatal Care, 18(3), 189-198.
2017
Lengerich, A., Bugajski, A., Marchese, M., Hall, B., Yackzan, S., Davies, C., & Brockopp, D. (2017). The Baptist Health nurse retention questionnaire: A methodological study, Part 1. Journal of Nursing Administration, 47(5), 289-293. doi:10.1097/nna.0000000000000480
Bugajski, A., Lengerich, A., Marchese, M., Hall, B., Yackzan, S., Davies, C., & Brockopp, D. (2017). The importance of factors related to nurse retention: Using the Baptist Health nurse retention questionnaire, Part 2. Journal of Nursing Administration, 47(6), 308-312. doi:10.1097/nna.0000000000000486
Davies, C. C., Brockopp, D., Moe, K., Wheeler, P., Abner, J., & Lengerich, A. (2017). Exploring the lived experience of women immediately following mastectomy: A phenomenological study. Cancer Nursing, 40(5), 361-368. doi:10.1097/ncc.0000000000000413
Melton, L., Lengerich, A., Collins, M., McKeehan, R., Dunn, D., Griggs, P., . . . Bugajski, A. (2017). Evaluation of huddles: A multisite study. The Health Care Manager (Frederick), 36(3), 282-287. doi:10.1097/hcm.0000000000000171
Fultz, A., Walker, M., Lengerich A., Bugajski, A. (2018) Job satisfaction of medical imaging technologists: A current look at work environment, communication and leadership. Accepted in Radiologic Technology.
2016
Davies, C. C., Brockopp, D., & Moe, K. (2016). Astym therapy improves function and range of motion following mastectomy. Breast Cancer, 8(1), 39-45. doi:10.2147/bctt.s102598
Brockopp, D., Hill, K., Moe, K., & Wright, L. (2016). Transforming practice through publication: A community hospital approach to the creation of a research-intensive environment. Journal of Nursing Administration, 46(1), 38-42. doi:10.1097/nna.0000000000000294
Bugajski, A., Lengerich, A., McCowan, D., Merritt, S., Moe, K., Hall, B., . . . Brockopp, D. (2017). The Baptist Health high-risk falls assessment: One assessment fits all. Journal of Nursing Care Quality, 32(2), 114-119. doi:10.1097/ncq.0000000000000220
Honaker, J. S., Forston, M. R., Davis, E. A., Weisner, M. M., Morgan, J. A., & Sacca, E. (2016). The effect of adjunctive noncontact low frequency ultrasound on deep tissue pressure injury. Wound Repair and Regeneration, 24(6), 1081-1088. doi:10.1111/wrr.12479
Bragg, L., Bugajski, A., Marchese, M., Caldwell, R., Houle, L., Thompson, R., . . . Lengerich, A. (2016). How do patients perceive hourly rounding? Nursing Manage, 47(11), 11-13. doi:10.1097/01.NUMA.0000502807.60295.c5
2015
Weyl, H., Yackzan, S., Ross, K., Henson, A., Moe, K., & Lewis, C. P. (2015). Understanding colorectal screening behaviors and factors associated with screening in a community hospital setting. Clinical Journal of Oncology Nursing, 19(1), 89-93. doi:10.1188/15.cjon.89-93
Alaloul, F., Brockopp, D. Y., Andrykowski, M. A., Hall, L. A., & Al Nusairat, T. S. (2015). Quality of life in Arab muslim cancer survivors following hematopoietic stem cell transplantation: Comparison with matched healthy group. Supportive Care in Cancer, 23(7), 2157-2164. doi:10.1007/s00520-014-2583-7
Bradley, H., Cantrell, D., Dollahan, K., Hall, B., Lewis, P., Merritt, S., . . . White, D. (2015). Evaluating preceptors: A methodological study. Journal for Nurses in Professional Development, 31(3), 164-169. doi:10.1097/nnd.0000000000000166
Davies, C., Brockopp, D., & Moe, K. (2015). Test-retest and internal consistency of the disability of arm, shoulder and hand (DASH) outcome measure in assessing functional status among breast cancer survivors with lymphedema. Rehabilitation Oncology, 33(1), 28-31.
Lewis, C. P., Corley, D. J., Lake, N., Brockopp, D., & Moe, K. (2015). Overcoming barriers to effective pain management: The use of professionally directed small group discussions. Pain Management Nursing, 16(2), 121-127. doi:10.1016/j.pmn.2014.05.002
Moe, K., Brockopp, D., McCowan, D., Merritt, S., & Hall, B. (2015). Major predictors of inpatient falls: A multisite study. Journal of Nursing Administration, 45(10), 498-502. doi:10.1097/nna.0000000000000241
Hahn, J., Byrd, R., Lengerich, A., Hench, J., Ford, C., Byrd, S., Stoltz, R. (2015). Neonatal abstinence syndrome: The experience of infant massage. Creative Nursing, 22(1), 45-50 6p. doi:10.1891/1078-4535.22.1.45
2014
Schreiber, J. A., Cantrell, D., Moe, K. A., Hench, J., McKinney, E., Lewis, C. P., . . . Brockopp, D. (2014). Improving knowledge, assessment, and attitudes related to pain management: Evaluation of an intervention. Pain Management Nursing, 15(2), 474-481. doi:10.1016/j.pmn.2012.12.006
Corley, D., Brockopp, D., McCowan, D., Merritt, S., Cobb, T., Johnson, B., . . . Hall, B. (2014). The Baptist Health high risk falls assessment: A methodological study. Journal of Nursing Administration, 44(5), 263-269. doi:10.1097/nna.0000000000000065
Davies, C., Nitz, A. J., Mattacola, C. G., Kitzman, P., Howell, D., Viele, K., . . . Brockopp, D. (2014). Practice patterns when treating patients with low back pain: A survey of physical therapists. Physiotherapy Theory Practice, 30(6), 399-408. doi:10.3109/09593985.2013.877547
Honaker, J., Brockopp, D., & Moe, K. (2014a). Development and psychometric testing of the Honaker suspected deep tissue injury severity scale. Journal of Wound Ostomy Continence Nursing, 41(3), 238-241. doi:10.1097/won.0000000000000024
Honaker J., Brockopp D., Moe K. (2014b). Suspected deep tissue injury profile: A pilot study. Advanced Skin Wound Care. 27(3):133-40; quiz 141-2. doi: 10.1097/01.ASW.0000443267.25288.87.
Kjelland, K., Corley, D., Slusher, I., Moe, K., & Brockopp, D. (2014). The best for baby card: An evaluation of factors that Influence Women’s Decisions to Breastfeed. Newborn & Infant Nursing Reviews, 14(1), 23-27. doi:10.1053/j.nainr.2013.12.007
Lewis, C.P. (2014). Knowledge development: Building on a solid foundation. Clinical Scholars Review for DNP. 7(1), 48-51.
Roser, L. P., Piercy, E. C., & Altpeter, T. (2014). Targeting zero: One hospital's journey to reduce CAUTI. Nursing Management, 45(12), 18-20. doi:10.1097/01.NUMA.0000456652.02404.b5
Stoltz, R., Byrd, R., Hench, A. J., Slone, T., Brockopp, D., & Moe, K. (2014). Does the type of sleep surface influence infant wellbeing in the NICU? MCN The American Journal of Maternal Child Nursing, 39(6), 363-368. doi:10.1097/nmc.0000000000000078
Thompson, M., Moe, K., & Lewis, C. P. (2014). The effects of music on diminishing anxiety among preoperative patients. Journal of Radiology Nursing, 33(4), 199-202. doi:10.1016/j.jradnu.2014.10.005
Watkins, S., Corley, D., Cleeter, D., Moe, K., & Brockopp, D. (2014). Implementing a nurse leader
fellowship model. Nursing Management, 45(7), 53-55. doi:10.1097/01.NUMA.0000451038.15082.b7
2013
Brockopp, D. Y., Moe, K., Corley, D., & Schreiber, J. (2013). The Baptist Health Lexington evidence-based practice model: A 5-year journey. Journal of Nursing Administration, 43(4), 187-193. doi:10.1097/NNA.0b013e31828958e7
Davies, C., Brockopp, D., & Moe, K. (2013). Internal consistency of the disability of arm, shoulder and hand (DASH) outcome measure in assessing functional status among breast cancer survivors. Rehabilitation Oncology, 31(4), 6-12.
Gilbert, P., Rutland, M. D., & Brockopp, D. (2013). Redesigning the work of case management: Testing a predictive model for readmission. The American Journal of Managed Care, 19(10 Spec No), eS19-eSP25.
Honaker, J. S., Forston, M. R., Davis, E. A., Wiesner, M. M., & Morgan, J. A. (2013). Effects of non contact low-frequency ultrasound on healing of suspected deep tissue injury: A retrospective analysis. International Wound Journal, 10(1), 65-72. doi:10.1111/j.1742-481X.2012.00944.x
2012
Honaker, J. S., Forston, M. R., Davis, E. A., Wiesner, M. M., & Morgan, J. A. (2013). Effects of non contact low-frequency ultrasound on healing of suspected deep tissue injury: A retrospective analysis. International Wound Journal, 10(1), 65-72. doi:10.1111/j.1742-481X.2012.00944.x
Schreiber, J. A., & Brockopp, D. Y. (2012). Twenty-five years later--what do we know about religion/spirituality and psychological well-being among breast cancer survivors? A systematic review. Journal of Cancer Survivorship, 6(1), 82-94. doi:10.1007/s11764-011-0193-7
2011
Blair, M., Hill, K. S., Walters, B. J., Senn, L., & Brockopp, D. A. (2011). Caring for nurses: Hospital-based study groups for certification. Journal for Nurses in Staff Development, 27(4), 165-169. doi:10.1097/NND.0b013e3181a68aae
Brockopp, D., Schreiber, J., Hill, K., Altpeter, T., Moe, K., & Merritt, S. (2011). A successful evidence-based practice model in an acute care setting. Oncology Nurse Forum, 38(5), 509-511. doi:10.1188/11.onf.509-51
Honaker, J., & Forston, M. (2011). Adjunctive use of noncontact low-frequency ultrasound for treatment of suspected deep tissue injury: A case series. Journal of Wound Ostomy Continence Nursing, 38(4), 394-403. doi:10.1097/WON.0b013e31821e87eb
Lewis, D. A., Sanders, L. P., & Brockopp, D. Y. (2011). The effect of three nursing interventions on thermoregulation in low birth weight infants. Neonatal Network, 30(3), 160-164. doi:10.1891/0730-0832.30.3.160
2010
Davies, C. C., & Brockopp, D. Y. (2010). Use of ASTYM® treatment on scar tissue following surgical treatment for breast cancer: A pilot study. Rehabilitation Oncology, 28(3), 3-12.
2008
Ross, K., Mathis, S., & Brockopp, D. (2008). Developing a successful palliative care service in an acute care setting. Journal of Nursing Administration, 38(6), 282-286. doi:10.1097/01.NNA.0000312787.88093.ca
Nursing Contributions to the Community
Baptist Health Lexington encourages nursing at all levels to volunteer and support community healthcare outreach programs and population health initiatives. Being a part of these events allows us to partner with community members and leaders while supporting improvements in public health. Activities may include health screenings, providing essential education, and linking patients to vital healthcare resources. Below are all the initiatives in which nursing professionals have participated over the last 24 months:
- Lexington-Fayette Urban County Government Employee Flu Vaccine Clinics
- Stroke Service Community Education initiatives for “BE FAST” – s... factors for stroke: Afib, HTN, DM, HLD, obesity, and nutrition:
- Woodhill Community Center and Urban Impact
- The Lexington School
- Educational presentations for hospitals across Kentucky on AHA g... transfer programs, and EMS/pre-hospital care of stroke patients
- Cancer Services initiatives include:
- American Cancer Society Belles and Beaus Ball
- Being Mortal – Advance Directive
- Breast, Colon and Lung Cancer Awareness
- Empowerment Series Women’s Cancer Support Group
- Hope Lodge
- Kentucky Cancer Link- Regional Colon Cancer Screenings
- Leukemia and Lymphoma Society – Light the Night
- Ovarian Cancer Awareness
- Race for the Cure
- Shine a Light on Lung Cancer
- Susan G. Komen Financial Toxicity Program
- Turn the Town Teal – Ovarian Cancer Awareness
- Ironcology
- DiverCity
- Lexington Community Health Fair education
- KyCancerLink
- Survivorship celebration Day
- Lexington pools skin cancer screening
- Metastatic Breast Cancer Support Group
- Oncology Patient Advisory Group
- Diabetes Services initiatives:
- CommUNITY Fest, (UnitedWay, St Martin Village Neighborhood Assoc)
- State of Diabetes Event, Regional ADA National Diabetes Month awareness presentation open to the public/payers
- Dixie Elementary Health Fair
- Ezra Sparrow Early Childhood Center Career Day
- UKFCU employee health fair
- Chronic Disease Awareness Booth
- Gray Health Fair
- FCPS Admin – Muscle Matters Series
- FCPS Admin – Fitness Friday Health Fair
- Fayette Co Diabetes Expo
- Baptist Health HealthTalks Podcast
- Baptist Health Bariatrics Facebook Live
- Salvation Army Nutrition Clinic
- Cardiovascular Service Initiatives:
- Mended Hearts Support Group
- Early Heart Attack Care and Hands-Only CPR education:
- Woodland Community Center and Urban Impact
- Dixie Elementary
- Commonwealth Credit Union
- Lexington Chamber Chorale Reception
- Warner Elementary School
- Kentucky Heart Disease and Stroke Prevention Task Force
- Chronic Disease Awareness Month
Reference:
Brockopp, D., Hill, K., Bugasjki, A. & Lengerich, A. 2018. Establishing a Research Friendly Environment: A Hospital-Based Approach. Boston MA: Jones Bartlett Learning
Institute of Medicine (IOM). 2011. The Future of Nursing: Leading Change, Advancing Health. Washington, DC: The National Academies Press. https://doi.org/10.17226/12956.



