What Is Osteopenia?
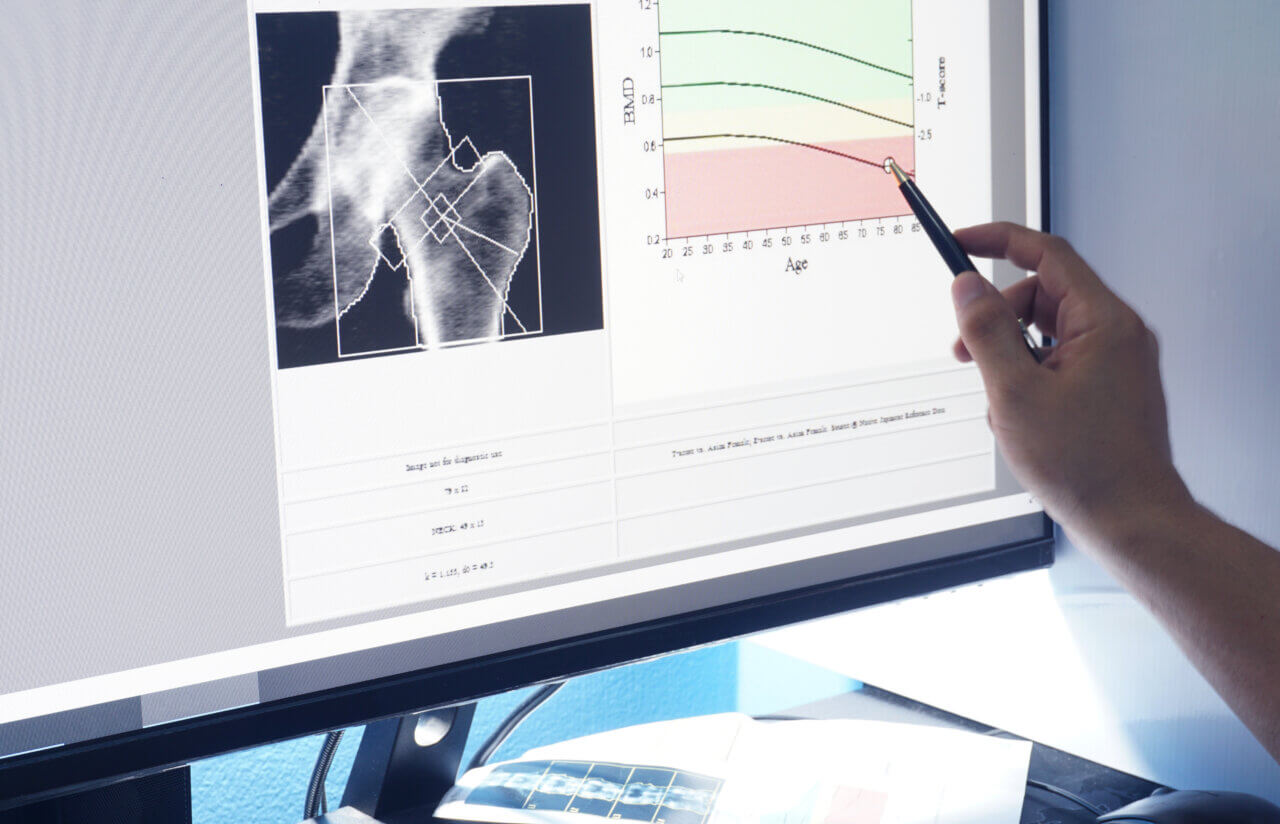
Most people associate low bone mass with osteoporosis. It’s a disease characterized by a drastic loss in bone density that causes bones to become brittle and fragile.
A lesser-known but related condition is called osteopenia. It affects nearly half of adults over 50. Osteopenia involves bone densities that are at less than peak levels but haven’t reached the point of osteoporosis.
This condition, and consequently osteoporosis, is more common in women than men, as females start with peak bone density levels that are much lower.
Osteopenia vs. Osteoporosis: Progression and Risk Factors
Osteopenia doesn’t always lead to osteoporosis. However, it can be a precursor to the disease. Consequently, learning about common risk factors associated with low bone mass is helpful.
If you or your doctor identify them, you can make appropriate diet and lifestyle modifications. These changes can help prevent or slow the loss of bone mass and the onset of osteoporosis.
Common low bone mass risk factors/causes include:
- Calcium or vitamin D deficiencies
- Lack of weight-bearing exercise
- Poor nutrition
- Alcohol abuse
- Smoking
- Drinking excessive amounts of soda
- Eating disorders
- Medical conditions including hyperthyroidism, Cushing’s syndrome, hyperparathyroidism, lupus, rheumatoid arthritis, and Crohn’s disease
- Radiation exposure
- Hormonal changes during menopause
- Chemotherapy
- Family history of low bone mineral density (BMD)
- Being older than 35
- Gastrointestinal surgery, which can affect nutrient and mineral absorption
- Taking prednisone or phenytoin
Osteopenia Symptoms and Diagnosis
Bone density naturally declines with age, but osteopenia typically has no symptoms. Many people only become aware of their low bone mass when they suffer unexpected fractures.
Fortunately, BMD testing (performed using dual-energy X-ray absorptiometry or DEXA) can help diagnose these conditions, enabling patients to take action to address them.
Experts recommend testing if you meet any of these criteria:
- You’re a woman who is 65 or older.
- You’re under 65, postmenopausal, and have any osteopenia risk factor.
- You’re postmenopausal and have broken a bone while performing normal daily activities.
Osteopenia Prevention and Treatment
It’s best to keep osteopenia from developing. You can reduce your risk by taking these actions:
- Following a nutritionally balanced diet that includes proper daily values of calcium and vitamin D
- Exercising regularly with weight-bearing activities
- Limiting consumption of alcohol and soda
- Eliminating tobacco use
If osteopenia or osteoporosis runs in your family, or you have one or more of the common risk factors, discuss your bone health with your primary care physician. If your doctor determines that you have osteopenia, they may recommend the following:
- Starting an osteopenia diet that increases your intake of vitamin D and calcium (including orange juice, vitamin-fortified breads and cereals, dried beans, spinach, broccoli, and wild-caught salmon)
- Safe sun exposure to help your body produce vitamin D
- Taking vitamin D and calcium supplements if necessary (intake from food is preferred)
- Increasing the amount of weight-bearing exercise you get daily
With proper diet and exercise, patients can stabilize their osteopenia and possibly even improve it. The key is to identify the condition early and address it.
If you have osteopenia or osteoporosis, you should also take action to minimize your risk of falls at home. This includes having adequate lighting to see tripping/slipping hazards, putting railings in showers and other areas, using non-skid rugs, etc.
Learn More About Osteopenia from Baptist Health
Osteopenia is a condition that puts you at risk of injury and may increase your likelihood of developing osteoporosis. Learn more about osteopenia on the Baptist Health website or talk with your Baptist Health doctor.
If you don’t have a primary care physician, locate one near you using our online provider directory.
Next Steps and Useful Resources
Menopause and Bone Loss: Preventing Postmenopausal Osteoporosis
What Is Osteoporosis?
Boost Your Bone Health Early



