Mammograms: Know When to Go
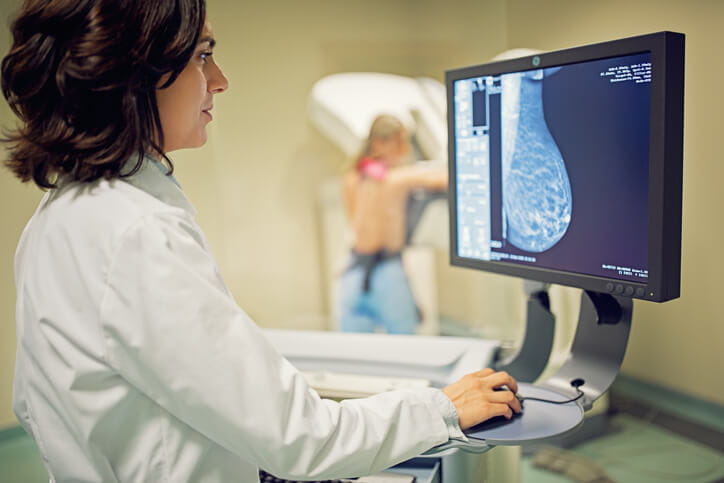
Schedule a Mammogram
Major medical organizations debate the exact age, but Angela Moore, MD, doesn’t share the confusion.
The medical director of Baptist Health Breast Imaging in Lexington sees no reason for women to deviate from what has long been the norm: yearly mammograms starting at age 40 for those at average risk of breast cancer.
In recent years, other recommendations have gotten fuzzy. The biggest shift came from the U.S. Preventive Services Task Force, which now recommends mammograms every two years starting at age 50. Even the American Cancer Society now says annual screenings can start later than it previously urged, at age 45 instead of 40.
Holding to the idea of annual mammograms beginning at 40 is the American College of Radiology, a recommendation endorsed by the Society of Breast Imaging.
Dr. Moore simplifies it: Go at 40 and go every year.
“I don’t understand the push to not have 40-year-olds screen for breast cancer,” Dr. Moore says. “We often see ladies who come in on the first screening and have cancer that was not detected clinically,” meaning during a manual examination.
In fact, early detection may be especially important for younger women, she says.
“Women in their 40s do benefit from early detection of cancer,” Dr. Moore says. “That’s a time when breast cancers may develop more rapidly.”
So why the delayed recommendations? Costs — both financial and mental —are a big factor. In their 40s, women tend to have denser breasts that raise more red flags, prompting follow-up exams that can include additional mammography or ultrasound tests. Much of the time the abnormalities turn out to be benign, and women get stressed out for nothing.
But the denser breast tissue that spurs more follow-up testing also provides another argument in favor of earlier screenings. Denser breasts are more likely to obscure an abnormality during a physical exam, while a mammogram “sees through” the tissue.
For all mammography patients, Baptist Health uses 3-D imaging, a technology that captures images in a way that allows the radiologist to examine small segments more closely. One technologist likened the technique to viewing an individual playing card pulled from the deck. The radiologist’s ability to study individual sections can sometimes eliminate the need for a follow-up visit.
Besides regular mammograms, Dr. Moore encourages women to be aware of their breasts, noting that experts have moved away from the idea of monthly self-exams, which are not a reliable screening tool.
“The encouragement now is for you to have breast awareness so that you’re aware of what’s normal for your breast, and if you notice a change, then you would seek attention for that,” she says.
Dr. Moore knows women — with families, careers, and homes to tend — often take care of themselves last. And she acknowledges that even she has let life get in the way, letting more than a year pass between mammograms.
But it’s best for women to take the time for the annual check.
“Breast cancer is treatable. But the time to catch it is before you feel it.”
Learn More About Your Risk and Find a Provider With Baptist Health
Assess your health and breast cancer risk with a free online assessment. Find a provider near you at BaptistHealth.com/provider.



