Be Smart About Antibiotic Usage
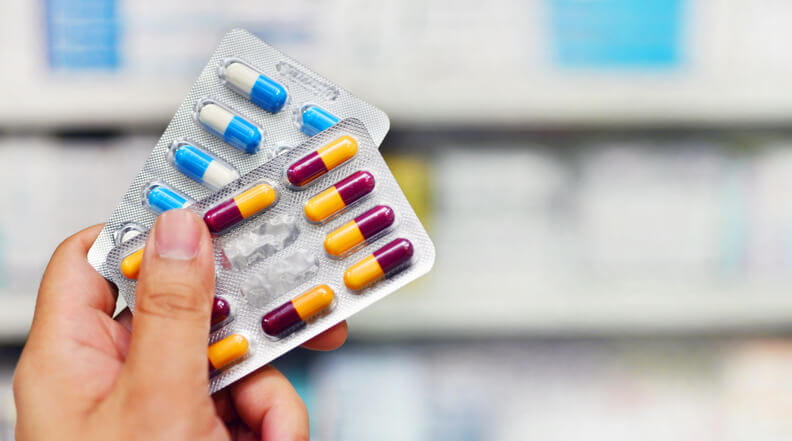
In the United States every year, at least 2 million people are infected with bacteria that are resistant to antibiotics and at least 23,000 people die as a direct result of these infections.
Thinking about taking antibiotics? Things to understand:
Bacteria are living organisms, and some bacteria cause infection. Sometimes your body’s immune system can get rid of infection on its own. Other times, antibiotics can help.
“Antibiotics are medicines that work either by killing the bacteria or by stopping the bacteria from multiplying, said Angela Sandlin, Pharmacy director at Baptist Health La Grange. “When antibiotics were first developed, infections that were previously deadly, such as pneumonia and cholera, became easily curable. People learned that infections were treatable with drugs, and unfortunately began to ‘expect’ to be treated with an antibiotic every time they had an infection.”
This expectation, along with a lack of understanding about resistance, led to antibiotic overuse. This repeated exposure to antibiotics causes some bacteria to become resistant and develop the ability to defeat the medicine designed to kill them.
Issues Surrounding Misuse and Overuse of Antibiotics
Some development of resistance to antibiotics is expected, but in recent years, the problem has been growing at an alarming rate. The misuse and overuse of antibiotics is the single most important factor leading to antibiotic resistance. Antibiotics are among the most commonly prescribed drugs, and — when used appropriately — these drugs are life-saving. However, up to 50 percent of all the antibiotics prescribed are not needed or are not optimally effective as prescribed.
An example of overuse is taking antibiotics for viral infections. Antibiotics are not effective against viruses such as the common cold, flu, most sore throats, bronchitis, and many sinus and ear infections. In viral infections, the antibiotic can actually be harmful. Certain bacteria live in and on our bodies, for example, on our skin, and in our intestines, and perform useful functions. When this “normal flora” of bacteria is unnecessarily exposed to the antibiotic, they may be killed, which can lead to side effects such as diarrhea, or even develop resistance to the antibiotic, causing problems later on when the antibiotic is truly needed.
Examples of misuse include not taking antibiotics correctly (missing doses), not finishing the whole amount that was prescribed, saving some for later, or sharing antibiotics with others. This misuse gives the bacteria a chance to develop resistance — not taking the full amount allows the more resistant bacteria to survive, then multiply, which can cause the infection to come back worse than before!
“As a country, and worldwide, we have overused and misused antibiotics to the point where some experts believe ‘we are at the end of the antibiotic era’,” said Sandlin.
Additionally, fewer antibiotics are in development. In order to help ensure there are antibiotics available for us and our children, we need to help prevent antibiotic resistance by “outsmarting” the bacteria.
3 Tips to Help Prevent Antibiotic Resistance:
- Prevent infections — wash your hands and get recommended vaccinations.
- Collaborate with your healthcare professional — do not “insist” on getting an antibiotic every time you or your child are sick. Explain that you are concerned about antibiotic resistance, and ask if an antibiotic is needed, or if there are steps you can take to feel better and get symptom relief without antibiotics. Sometimes antibiotics are necessary, even life-saving. Talk with your healthcare professional to decide what is best.
- If an antibiotic is needed, take it exactly as prescribed — do not skip doses, and take it for the full number of days prescribed, even if you are feeling better. Failure to take the whole amount can cause the infection to come back and be much worse and harder to treat. Do not save some pills for next time, or share some with others. Never take antibiotics that were prescribed for someone else.
 Angela Sandlin
Angela Sandlin
Angela Sandlin, Pharmacy director at Baptist Health La Grange.